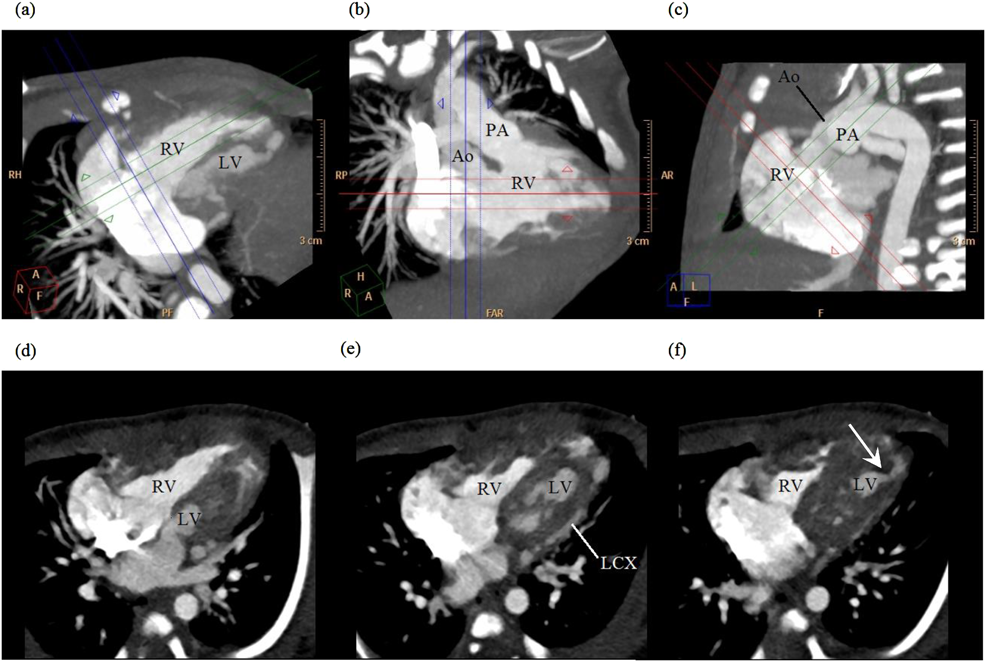
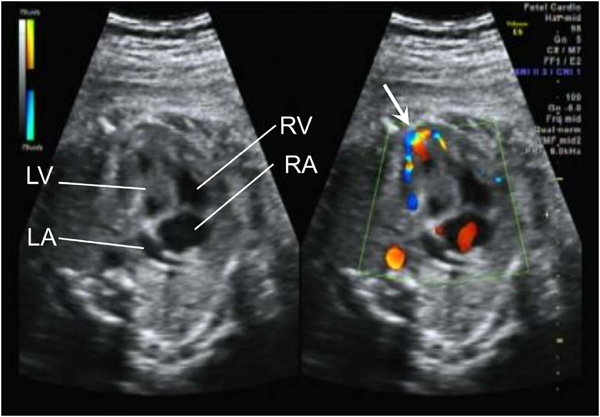
Successful Staged Fontan Completion for Double-outlet Right Ventricle with Intact Ventricular Septum
1 Department of Pediatrics, Fukui Cardiovascular Center ◇ Fukui, Japan
2 Department of Pediatrics, Municipal Tsuruga Hospital ◇ Fukui, Japan
3 Department of Pediatrics, Fukui Aiiku Hospital ◇ Fukui, Japan
4 Department of Cardiovascular Surgery, Fukui Cardiovascular Center ◇ Fukui, Japan
5 Department of Pediatric Cardiovascular Surgery, Children’s Medical Center, Kyoto Prefectural University of Medicine ◇ Kyoto, Japan