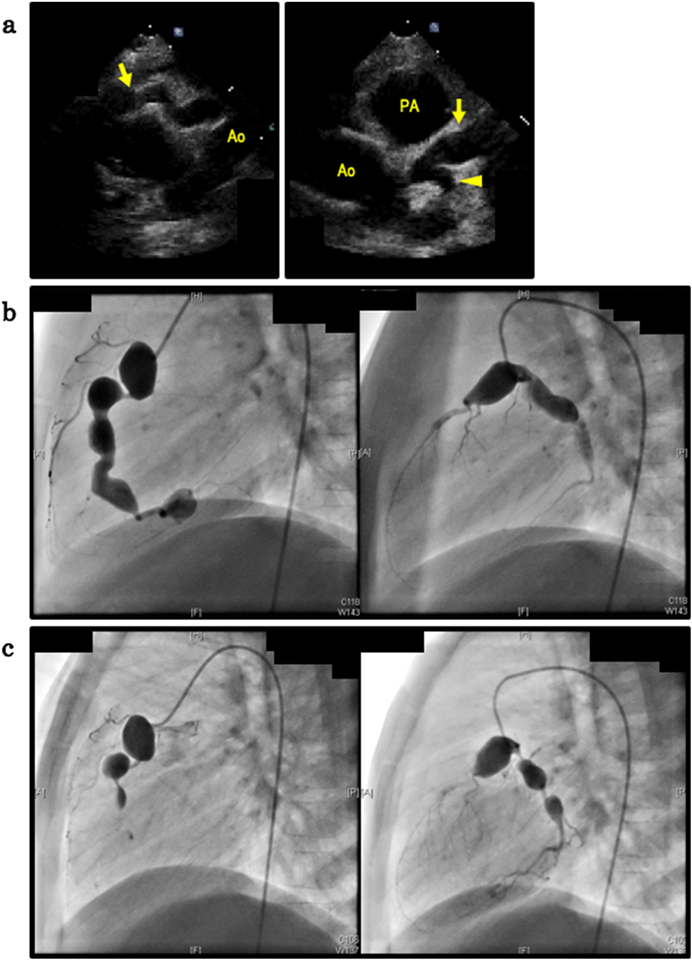
Multiple Giant Aneurysms at Both the Right and Left Coronary Arteries in Incomplete Kawasaki Disease
1 Department of Postgraduate Education and Training, National Center for Child Health and Development ◇ Tokyo, Japan
2 Division of Cardiology, National Center for Child Health and Development ◇ Tokyo, Japan
3 Department of General Pediatrics and Interdisciplinary Medicine, National Center for Child Health and Development ◇ Tokyo, Japan
4 Department of Management and Strategy, Clinical Research Center, National Center for Child Health and Development ◇ Tokyo, Japan
5 Department of Pediatrics, Saiseikai Yokohamashi Tobu Hospital ◇ Kanagawa, Japan
6 Department of Pediatrics, Kawakita General Hospital ◇ Tokyo, Japan
7 Noma Pediatric Clinic ◇ Tokyo, Japan